
|
|||||||
Scoliosis
What is it?
Scoliosis is a condition where the spine is curved sideways. To clarify the concept, the reader should note that this is different from kyphosis, where the spine is curved forward (as in round-back), and lordosis, where the spine is curved backward (as in sway-back).
What causes it?
Scoliosis can be non-structural and caused by factors unrelated to the spine, e.g., poor posture, leg length discrepancy, back muscle spasm. The scoliosis disappears once the cause is removed.
Scoliosis which is structural is usually due to a cause that resides within the spine, even though it may initially have started somewhere else. For example, neuromuscular problems like muscular dystrophy and poliomyelitis cause muscle imbalance, which initially cause a non-structural scoliosis. Over time, however, secondary changes occur in the spine which then lead to a structural scoliosis.
Scoliosis due to problems in the spinal column include congenital defects of spine development like congenital hemivertebra, where one half of the vertebral body fails to develop. With asymmetric growth, scoliosis is bound to develop. In other instances, two or three vertebral bodies during development stays unsegmented. If only one half of the vertebral bodies stay unsegmented, symmetric growth and scoliosis will develop. While congenital scoliosis (due to vertebral abnormalities) are serious problems that often require early surgery, they are rare.
The commonest form of structural scoliosis encountered is Idiopathic scoliosis. Idiopathic scoliosis can occur during the first 3 years of life (called Infantile idiopathic scoliosis), from 4 to 10 years of age (called Juvenile idiopathic scoliosis), or from 10 to 15 years of age (called adolescent idiopathic scoliosis). Adolescent idiopathic scoliosis, which occurs during puberty, is by far the commonest type of structural scoliosis encountered.
As the word "idiopathic" suggests, no one exactly knows why it occurs. It is well known to occur during the growth spurt of puberty, especially in girls. It also tends to run in families, suggesting a multifactorial hereditary predisposition. Studies have shown biochemical changes in the vertebral bodies, the disc material, and even the paraspinal muscles. But one cannot be sure if these cause the scoliosis, or are changes that develop secondary to the scoliosis.
The following discussion will concern itself with idiopathic scoliosis.
What are the symptoms?
Scoliosis does not cause pain in the growing child, so it was not unusual to be discovered only when the curvature was obvious, and severe. The observant teenager, or parent, may notice the shoulders and pelvis not being level while the child is standing. Or the patient may notice that her breasts are not quite symmetrical, or her bra does not fit too well.
More recently, with routine school screening, many children are referred with very early curves. This has been a great advance, because early treatment can be instituted. The education that goes with the school screening also creates greater awareness of the problem, and encourages the child to talk about it if she suspects a problem. The danger, of course, is unnecessary X-rays and/or treatment in the hands of inexperienced or unscrupulous practitioners.
How do you prevent it?
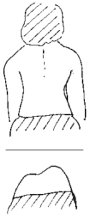
Since no one knows the exact cause of idiopathic scoliosis, prevention is not possible. But recent school screening programs have helped in detecting early cases with timely referrals. You can screen your child for scoliosis very easily by having your child bend forward away from you with her hands together and arms hanging freely in front of her body. Scan the profile of her back while she is bent forward to check for any asymmetry.
What does your doctor do about it?
Your doctor will take a detailed history and perform a careful examination to determine the severity of the curvature, as well as to rule out any underlying cause for the scoliosis, before labelling it "idiopathic". He will have your child bend forward away from him, and check for any asymmetry as described above. He will use an instrument called a Scoliometer to measure the angle of trunk rotation (ATR). An ATR of 7 degrees or more requires an X-ray.
He will order a standing X-ray of your child�s spine, to check the alignment of the spine, and measure the extent and angle of the curvature. The severity of the scoliosis is expressed as angle of curvature, using a measuring technique on the X-ray film, known as the Cobb method. From the X-rays, your doctor will be able to assess the maturity of the spine, and if there is still any more growth left to the spine. This has great significance for prognosis, since the scoliosis can get worse with growth. If the curve is severe enough, he may also do side-bending X-rays to assess the rigidity of the curve. Occasionally, he may order an MRI if he suspects any underlying problem in the spinal cord.
The decision to treat depends on several factors. Firstly, you need to realize that once a child has scoliosis, she will continue to have it. The scoliosis does not revert to "normal". Secondly, most curves are mild (less than 20 degrees) and stay mild. These do not cause any medical or cosmetic problems, and are best left alone. If your doctor discovers you have a scoliosis of less than 20 degrees, he will probably not recommend any treatment, other than regular checkups and observation. If your child is prepubertal, the doctor may see her just once a year, and perform annual X-rays as necessary to check on the curve. If your child is an adolescent, and in the midst of a growth spurt, the chances of the curve worsening is higher. Your doctor will need to see her every 3 or 6 months to check on the curve. Once growth is completed at age 15 or so, the curve is unlikely to worsen. If the curve is less than 20 or 25 degrees at age 15, it is likely that your child will continue to have a scoliosis that will not affect her life in a significant way.
If your child is discovered to have a curvature more than 25 degrees, or subsequently develops the curvature on follow-up, treatment will be needed. At this stage, treatment consists of bracing. It is found that curvatures of this magnitude, especially in a younger child, tends to be progressive. Bracing does not straighten a curve. The purpose of bracing is to prevent the curve from getting worse.
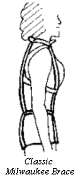
The classic brace that has been used since the 1950�s is the Milwaukee brace (developed by Drs. Blount and Schmidt from that city). It consists of two metal struts that extend from the occiput and chin to the pelvis, and a series of cleverly placed corrective pads along the torso. The braces were worn 23 out of 24 hours a day. Though effective, it was very punishing to a self-conscious adolescent girl, and compliance was a problem.

Mercifully, treatment has evolved over the last few years, to use of an underarm brace that extends from the axillae to the hips. The brace is made of thermoplastic material, with corrective pads incorporated in the brace. Although not suitable for every patient, depending on the level of the curve, the brace is much more comfortable. The good news about brace wear is that recently, it has been found that wearing the brace for 16 hours a day is good enough for curve control. This allows the patient to be off the brace for 8 hours a day, and she can decide the most advantageous time to do that!
Activity is encouraged during brace wear, and your child can participate in most activities, with the exception of contact sports.
Whatever brace your doctor chooses for your child, brace treatment is needed till growth is complete, around age 15. During the last year of treatment, your child will be weaned off your brace, wearing it for less hours every three months or so.
If bracing fails to control the scoliosis, and the angle of the curve gets beyond 40 to 45 degrees, surgery may be needed. Surgery consists of fusing the curved portion of the spine, which stops the curve from getting worse, but also stops its growth. Hence, it is important to try to postpone the surgery as long as possible. In young children, where the curve is so severe that waiting is not feasible, a limited fusion may be done.
In the past, when surgery is contemplated, the patient is placed on a special table that allows some correction of the scoliosis. A body cast is then applied. A large window is then made in the back, and surgical fusion is then performed while the patient is in the cast. Following the surgery, the cast is worn for at least 6 months. What agony! Great strides have been made in the surgical treatment of scoliosis in recent years. Advances in surgical hardware now makes it possible to perform the correction right on the surgical table, as well as hold the correction while the spine fuses. The Harrington rod (with posterior fusion) was the first in a series of innovative implantable hardware that started this revolution. More recently, the Cotrel-Dubousset (French) and the Texas Scottish Rite Hospital systems are being increasingly used. These involve fusing the spine posteriorly and anteriorly (a much bigger operation), but have the advantage of not needing any post-operative bracing or casting. There are significant risks involved, including paralysis from injury to the spinal cord during the surgery. For the right patient, the results are well worth the risks.
What can be expected after treatment?
To put things in perspective, most curves are mild (less than 20 degrees) and non-progressive., and do not require treatment. Of those that require treatment, bracing does the job. Only in a minority of patients will surgery be needed.
If a progressive curve is untreated, severe deformity can result. The more severe thoracic curves can impinge on lung reserves, and cause cardio-respiratory problems. By treating a progressive curve early can prevent these complications from happening.
Treatment for scoliosis, whether by bracing or surgery, is a long-term project. It requires teamwork involving your doctor, the parents (or guardians) and the patient. The patient has to understand why he or she needs treatment, and be motivated to undergo treatment, for it to be a success.
NOTICE: The information presented is for your information only, and not a substitute for the medical advice of a qualified physician. Neither the author nor the publisher will be responsible for any harm or injury resulting from interpretations of the materials in this article.
Questions
or comments? Post your thoughts in the Orthoseek
Message Forum!
Find a pediatric orthopedic surgeon
in an area near you.
Home | About Us | Orthopaedic Topics | Message Forum
![]()
Comments, questions, or suggestions are welcome. Please
contact us using this form.